Written by Malman Law, reviewed by Steve J. Malman.
Bedsores, also known as pressure ulcers, are not an annoyance; they are a severe health and safety risk that are entirely preventable.
Bedsores affect those who are confined to the same position for long periods, especially comatose patients who cannot reposition themselves and rely solely on their caretakers for movement. Pressure ulcers can happen if there is friction or pressure on a specific area of the body (usually bony areas), and the sores continue to form if the patient is not repositioned.
Typically, pressure ulcers form on elbows, knees, ankles, heels, and the lower back. They are entirely treatable, but also preventable. When a patient develops sores and those sores are allowed to remain untreated, the nursing home or individual responsible for caring for the patient can be held legally responsible for their actions.
Whether you have a loved one in a nursing home, hospital, or they are being cared for at home by a nursing service, there is no excuse for bed sores. Furthermore, there is no excuse for these sores to continue past Stage 1 where they pose serious health risks to the patient.
Intensive care units in the US see an average of 16.6 to 20.7 percent of their patients developing pressure sores. And because they are so common, it is imperative that family members be proactive and ensure their loved one is repositioned frequently to avoid them.
Certain risk factors increase the likelihood a patient will develop pressure ulcers, which include:
A patient in a coma has no mobility. Therefore, they are at high risk of developing bedsores because they cannot reposition themselves to avoid continuous pressure on the skin.
Certain health conditions might thin the skin, create blood circulation issues, or weaken a patient’s immune system – all of which can increase the chances of them developing pressure sores.
Comatose patients rely heavily on their caretakers to bathe them, change them, and clean them if they soil themselves. If a patient is allowed to remain soiled, urine and feces can degrade the skin and increase the risk of a pressure sore as well as become a serious infection if there is already an open sore present.
Pressure ulcers are preventable by following a few tips. Any nursing care facility that specializes in the care of a comatose patient should have protocols in place to inspect for and treat pressure sores (which can develop in a matter of hours) and to prevent ulcers from happening.
Some ways to prevent bedsores from forming include:
Comatose patients should be repositioned every couple of hours (sometimes as little as every 30 minutes) and throughout the day to reduce their risk of developing these sores. Repositioning might mean moving them from their back, to the right side, then to the left side, and so forth. Using pillows and propping devices will ensure that their weight does not drag them back down to a position that they were already in.
The cleaner the patient’s skin is, the less likely they are to develop an ulcer. Comatose patients should be bathed regularly using warm water and mild soap. Their skin must be pat dry because any moisture that remains can lead to sores, too. Frequently changing their bedsheets, inspecting for any leaks from the catheter, and changing diapers are equally important.
Some facilities implemented the use of water beds because they provide uniform pressure, but without pressure points being irritated. While these are expensive, they can be beneficial for those lying down for extended periods of time.
Using foam cushions under a patient might also provide equal pressure without irritating bony areas of the body.
Pillows can prevent bedsores by reducing pressure. For example, a comatose patient moved to their side can have a pillow placed in between their knees and ankles to reduce the burden on those bony points.
Comatose patients should still receive exercise. This includes helping move parts of their body to promote blood circulation and keep the muscles from weakening. Most hospitals use physiotherapy for their comatose patients a few times per week, including movement and massage.
Most comatose patients are kept in hospital gowns. But if they are dressed, avoid clothes that have buttons, zippers, or thick seams. Clothes should not be too tight either, because this can restrict blood flow.
Another preventative method is the use of an air mattress pad when foam or water beds are unavailable. The air mattress pad works similarly to waterbeds by creating equal pressure.
If proper prevention techniques are used and the patient still develops pressure ulcers, it is imperative that they are caught and treated right away. Once pressure ulcers reach a certain point, they become untreatable and fatal.
Bedsores have four distinct phases, with the first and second being the least dangerous while the third and fourth can be life-threatening.
Stage one sores are a mild irritation and sometimes missed by inexperienced caregivers. Those with experience caring for bedridden or comatose patients would recognize a stage one wound because they are trained to know what to look for.
Stage one sores affect the upper layers of the skin and have not entered deeper tissue or bone. The spot might feel different from the surrounding skin, such as being softer or firmer. It also might have a red irritation to it, but a full sore has not formed yet.
Stage one sores can clear up in two to three days with proper treatment. This is a critical time frame for caregivers to take proper measures to keep the sore from becoming worse.
By stage two, the sore has developed deeper in the skin layers. It is obvious there is a sore now because the skin is open and might even have a pus-filled blister. Around the sore, you may notice redness, warmth, and skin swelling.
Now is the time for the sore to be treated immediately. While it should have been caught and treated in stage one, stage two sores are apparent, even to the untrained eye. There is no excuse for not seeing these sores on a comatose patient.
Unfortunately, many nursing home patients do not receive the care they need, and eventually their stage two sore turns into stage three. Stage three sores move through the second layer of skin and enter the fat tissues.
Now the sore looks more like a crater, and it is likely infected at this point so a foul odor is present. Stage three sores cannot be treated by nursing home staff alone. Instead, they require physician intervention. Often antibiotics are necessary to treat underlying infections, and dead tissue around the sore is removed to prevent further tissue death.
Sadly, stage three sores will require daily care and take one to four months to heal, which means the chance of further infection is likely.
Stage four bed sores are the most serious and unnecessary. A pressure ulcer should never be allowed to progress to stage four where muscles, ligaments, fatty tissues, and skin are all affected. The infection is more likely to enter the blood at this point, resulting in sepsis and sometimes a more serious condition known as septic shock.
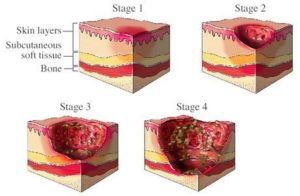
Photo Credit: Elizabeth Anderson Dermatology
Bone infections can also occur once the sore reaches stage four. Any stage four pressure ulcer requires hospital treatment. And most of the time, these wounds need surgical correction. Most stage four pressure ulcers take three months to a year to heal – sometimes longer if the patient has a health condition that affects circulation or their immune system.
In a nursing home setting, the patients there (including those who are comatose) have an expected standard of care. Their family has placed them in that nursing home under the assumption that, in return for payment, the nursing home staff will meet the daily care needs of their loved one. This includes repositioning throughout the day to avoid deadly bed sores.
When your loved one develops a bed sore due to inadequate staffing or they develop a life-threatening infection because nursing home staff failed to seek medical treatment, you have the right to hold the nursing home and their team responsible.
To explore your option and advocate for a loved one who cannot do so themselves, contact the attorneys at Malman Law.
We are here to fight for your right to compensation aggressively, and we hold nursing homes responsible so that patients under their care receive the treatment they deserve.
Schedule your free consultation now at 888-625-6265 or request further information about our services online.
Malman Law’s founder Attorney Steven Malman has over 30 years of experience handling personal injury, nursing home, medical malpractice, truck accidents, car accidents, premises liability, construction, and workers’ compensation cases in Chicago, IL.
Years of experience: +30 years
Illinois Registration Status: Active and authorized to practice law—Last Registered Year: 2024